On December 19, 2022, the OIG issued its annual report on Medicare lab spending. The headline is, "17% increase from 2020, driven by COVID-19, Genetic tests, Chemistry tests."
The report homepage is here. The 13-page PDF report is here.
These annual reports are required by the 2014 PAMA law. They include both Part B and hospital outpatient lab data; on the CMS website, it's easiest to find detailed Part B data alone.
Total lab spending was $9.3B in 2021. The report notes that "high priced genetic tests increased by 56%" and this category was $1.9B, up from $1.2B. The top 25 tests are 59% of dollar volume.
As I've belabored for several years, hundreds of millions of dollars of the genetic test spending are nonsensical claims from labs often indicted or convicted by DOJ, typically enormous claims volumes for multiple units of 81408 - rare gene full sequencing - which on their face, are inconsistent with any version of reality. Here. This large bolus of "extremely atypical" claims each year (including 2021) make calculations about actual growth rates in real patient care genomics difficult.
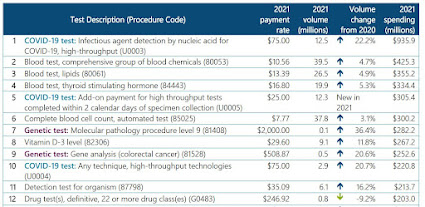
The fact that OIG drily notes on page 6 that 81408 rose 36% in 2021 and tallied $282M, should be a cause for shock and horror at CMS. This spending is 180 degrees in contrast with fraudulent spending, for example, on electric wheelchairs. A Medicare patient might, possibly, need an electric wheelchair so the claim (even if fraudulent) might be valid. In contrast, no Medicare patient has ever needed exactly 2 units of every Tier 2 genetic code from 81400 to 81408 - that's beyond nuts. Page 7 shows that 81408 was the highest-paid genetic test (and the 7th-highest of all tests of all types) - insanity is too weak a word.
Hospital claims are typically 20-40% of total claims for normal lab tests. For 81408, hospital claims contribution is essentially 0, because claims are from pop-up bizarrely unbelievable billing patterns in the Novitas and FCSO MACs.
 |
| click to enlarge |
