In the January 2022 issue of Health Affairs, Schwartz et al. study the rate of denials in Medicare Advantage, using Aetna data (most authors from CVS which acquired Aetna in November 2018). Denial rates were only about 1% and 85% of Medicare Advantage denials were rooted in Medicare fee for service policies. (Aetna can deny additional claims, when there is no Medicare policy to the contrary and when the service is deemed not beneficial by Aetna). Here.
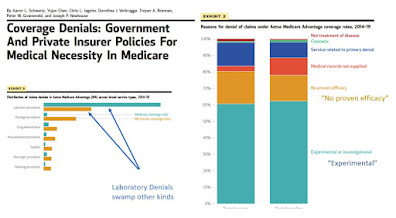
Of additional interest, Exhibit 2 in Schwartz et al. shows that 80% of denials were due to "experimental" or "no proven efficacy" while 10% were denied due to lack of medical records. Most of the remaining 10% were denied relative to some primary denial (e.g. if a surgery fee is not necessary, the anesthesia fee is not necessary).
Exhibit 3 shows that laboratory service denials swamp out all other medical service areas, which are miniscule in comparison.
Another interesting fact is that when there are Medicare Advantage denials for oncology or drugs or surgery, they are usually caused by Medicare Advantage rules. (Gold bar longer than the very short green bar). This is because FFS Medicare has few LCDs (or NCDs) on cancer care, or on other drugs, or surgeries.
 |
| Click to enlarge. |
For an article on rough-and-tumble contracting amongst MA plans, here.